Laura Mariana Amador-Castilla 1; Joaquín Javier Camacho-Tapia 1; María Esperanza Romero-Barrionuevo 1
1 Faculty of Medicine, University of Granada (UGR)
Translated by:
Graciela Isabel Piedra-Molina 2; Andrea Moreira-Piñero 2; Ana Rodríguez-Martín 2; Antonio Moral-Pulido 2; María Leonés-Alonso 2; Marta Mozola 2
2 Faculty of Translation and Interpreting, University of Granada (UGR)
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is the virus that causes the coronavirus disease 2019, also known as COVID-19. Over 900,000 people have died of COVID-19 in Europe since the beginning of the pandemic. The aim of this review is to analyze the impact of the pandemic on the mental health of doctors and nurses throughout Europe.
The studied risk factors were: being young, being female, the lack of adequate protective equipment and the fear of becoming infected and transmitting the virus to relatives, patients and colleagues. The most frequent protective factors were: the access to adequate protective equipment, knowing the protocols against COVID-19 and studying the disease. In general, there was an increase in anxiety, stress, insomnia, depression and even suicidal ideation.
The most frequent negative effects observed in doctors were guilt, confusion and exhaustion. However, the social recognition of their work had a very positive influence on them. As for nurses, several studies considered that they suffered more than doctors during the pandemic due to a closer contact with patients. However, the fact that they had to make a greater effort to care for patients increased their compassion satisfaction more than among doctors.
The COVID-19 pandemic has presented the health care system with a challenge. Stress and difficult decision making in extreme situations have had a negative impact on the mental health of doctors and nurses. Therefore, the implementation of measures that support their mental health is recommended.
The result is mostly consistent with a negative impact on the mental health of doctors and nurses. This is an issue that should be addressed in a more natural way within these groups. This would also benefit patients, because they would receive higher quality care.
Keywords: COVID-19, mental health, doctors, nurses, effects, risk factors.
Introduction
SARS-CoV-2 was first identified in December 2019 in Wuhan (China). This virus causes COVID-19 in humans. Due to its easy transmission and the lack of knowledge about the virus, it spread rapidly. Hardly three months later, on March 11 2020, the World Health Organization (WHO) declared COVID-19 a pandemic (1). In addition, the exponential increase of cases in Europe led this continent to become the new epicenter of the virus.
In Europe, since the beginning of the pandemic, 920,952 people have died as of March 25 2021 (2). The coronavirus has had multiple consequences, such as the economic, social and mental crises, while the number of cases increased until the health system was overloaded. Most of the measures aimed at reducing the transmission have focused on social distancing. As a result, a dehumanization of social relations has occurred, with the possible consequences that this might lead to (3).
The aim of this review is to study the impact of the pandemic on the mental health of doctors and nurses. At the same time, it seeks to examine protective factors in order to promote them. This will encourage good mental health among healthcare workers and will therefore result in a better patient care.
General factors affecting mental health
Several studies identified factors related to the impact of the COVID-19 pandemic on the mental health of healthcare professionals. These factors had to be classified due to their wide variety. (Table I) The following classification is proposed based on two criteria: 1) whether the factors have a negative or a positive effect (risk/protective factors) and 2) whether they are dependent on health professionals or not (dependent/independent factors). A factor is considered to be independent when it is beyond the control of the person it affects and a dependent factor is that determined by the person’s preferences or qualities. During the analysis and the categorization, some traits could not be easily classified. For these factors, an intermediate category called “hard-to-classify factors” was created.
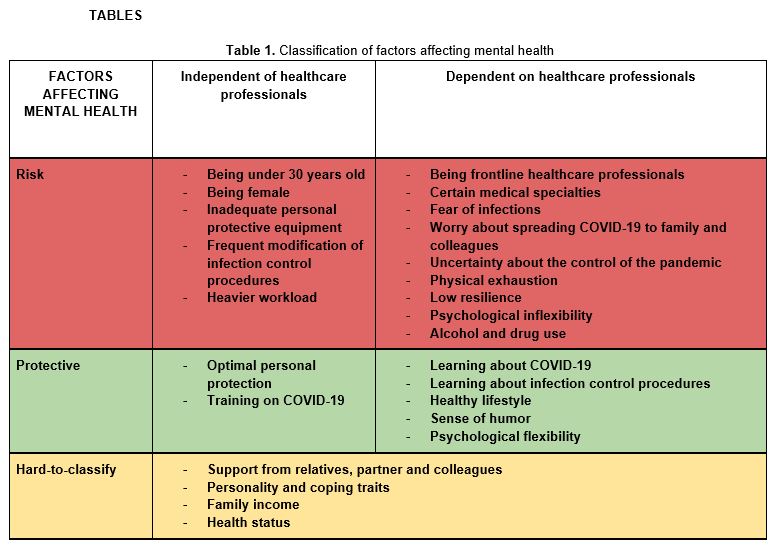
The independent risk factors were: being young, especially under thirty years (4-7); being female (8-10); the lack of adequate personal protective equipment (9, 11); the difficulty in remaining updated due to the frequent changes in infection control procedures (3, 12); and the increased workload due to the pandemic (9, 11).
The protective factors considered independent were: having optimal personal protective equipment and receiving training on protocols to combat COVID-19 (4, 13).
The risk factors classified as dependent were: working on the frontline (5); working in certain medical specialties (14), such as psychiatry (6), obstetrics, gynecology and traumatology (12, 15); the concern about becoming infected and, in particular, about infecting relatives, colleagues or patients (3, 16); the uncertainty about when and how the pandemic will end (3); the physical exhaustion due to the heavy workload (9, 11); the psychological inflexibility; the low resilience to cope with the consequences of their actions (6); and the use of alcohol and other drugs (3), although one study states that this was the least used coping strategy (13).
The more personal, dependent protective factors were: learning about COVID-19 and the infection control procedures on one’s own (3) and having a healthy lifestyle, sense of humor and psychological flexibility (6).
Mental health was also affected by factors that are more difficult to classify, such as the support from family, partners, friends and colleagues (17), the household income, the person’s health status and the personality and coping traits (18, 19).
General effects on the mental health of doctors and nurses
The rapid evolution of the pandemic and the uncertainty generated a high level of anxiety in the population, as well as in healthcare workers. According to studies conducted in previous pandemics such as the SARS pandemic, a potentially fatal disease could increase mental stress with physical and psychological consequences (8). Previous studies often include scales such as the COVID-19 Anxiety Scale (CAS), the Brief Resilience Scale (BRS) and the Clinical Outcome in Routine Evaluation-YP (CORE-YP) to ensure that the information collected is as objective as possible (20).
Most doctors were afraid of becoming ill and its consequences, such as infecting colleagues, the clinical sequelae of COVID-19, having to confine themselves or finding difficulties to return to work (16). However, these risks were regarded with resignation as part of their job (9). The fear of infecting relatives with SARS-CoV-2 is associated with increased anxiety, stress, insomnia and depression (8, 10, 21, 22). Other factors, such as the easy transmission of the virus (22-24), its high virulence (22, 25) and its great morbimortality increased fear, anxiety and even panic attacks (22, 26-28). Moreover, uncertainty is also having a negative impact on mental health (3).
The psychological impact was present even in countries with a relatively low number of COVID-19 cases (4). The most frequently observed effects were depression, anxiety and stress (3, 18). A meta-analysis covering data from 33,062 people showed a prevalence of 22.8%, 23.2% and 38.9% of depression, anxiety and insomnia in countries affected by COVID-19 (29). This was also the result of a study performed at the General Hospital Nasice (Croatia): 11% of the healthcare professionals suffered from moderate to very severe depression and the same happened with stress to 10% of them (30). However, most of the studies assessing mental disorders were conducted online, so they might have overestimated the prevalence of some of these disorders. This is due to the fact that the individuals who suffer the most from these disorders (depression, anxiety, burnout syndrome) are often the ones who answer these questionnaires the most (5, 31).
As for suicidal ideation, a study conducted in Cyprus in May 2020 showed that 6% of the healthcare workers had suicidal thoughts (4). Another study conducted in China revealed a similar percentage: 6.5% of the 8,817 healthcare workers participating in this study showed signs of suicidal ideation or self-harm (32). Technological development also had an impact. The population, that is, healthcare workers, are increasingly using social networks. The increased use of social networks, together with the infodemic, increased the feelings of anxiety and worry, which had a negative impact on mental well-being (33).
Healthcare workers who were on the frontline against COVID-19 generally showed an increase in depression and post-traumatic stress symptoms (10, 21, 22). This is due to the great responsibility they had to bear in extreme situations and to their long working hours (22). Moreover, a study conducted in Spain also found a relationship between the regions most affected by the pandemic and the prevalence of mental disorders. The mental well-being of healthcare workers varied depending on the number of deaths per day and the stage of development of the COVID-19 (17, 18). During the impact phase—the upswing of the epidemic wave of the new outbreak—, the stress level is even lower than in the disillusionment phase. The ability to face new epidemic waves will decrease if there is not enough time for psychological recovery (20). Even though having to face challenges such as COVID-19 brings out the best of these professionals, it also causes subsequent burnout syndrome and exhaustion. In addition, stress interferes with the feeling of satisfaction for the work carried out (34). Therefore, implementing measures that enhance the recovery of healthcare professionals will enable them to deal with a new outbreak in the best possible way (20).
In addition, the social recognition of the healthcare workers reduced the psychological effects of the pandemic to a certain extent, because it provided them with a sense of self-efficacy and with positive reinforcement (8). Humor was one of the most used measures to protect mental health among doctors and nurses. This reduced the negative impact of the pandemic (3, 6). Making people remember their beloved ones, together with the positive work-related thoughts, such as a sense of usefulness in the battle against the virus, can be beneficial for the emotional well-being and therefore for coping with stress.
Those who had previously shown psychological problems are at a higher risk in extreme situations such as this pandemic. Therefore, the early detection of psychological problems is important to identify the individuals at a higher risk and to be able to act on time (9). A study conducted in Belgium showed that between 18% and 27% of the health workforce required professional psychological help during the pandemic (17).
Although most of the gathered information supports that the COVID-19 pandemic had a negative influence on the mental health of healthcare workers, a few research articles claim the opposite. A study conducted in China found that burnout syndrome and exhaustion were less frequent among the healthcare workers who worked with COVID-19 patients than among those who worked in other areas (8, 35). Another study conducted in Germany revealed that these professionals presented lower anxiety and depression rates because they were more informed about COVID-19 than the rest of the population (20).
Other researchers investigated some parameters that analyze in detail the differences in the psychological impact between both sexes. Several studies indicate a higher prevalence of post-traumatic stress in women (than in men). In fact, the probability of experiencing post-traumatic stress is estimated to be between double and triple higher among women (8, 10, 36-39). The influence of their couple on the mental toughness of women has also been widely studied. Women per se are more liable to experience symptoms of depression, but single women are even more likely to develop these disorders (10, 40-42). Age does not seem to play an importantrole, but women aged between 30 and 49 experience the highest impact on their emotional well-being (10, 17, 36). In general, women, especially those who work in COVID units or in Intensive Care Units (ICU), present symptomatology and mental health disorders more frequently (9).
- Impact among doctors
Doctors are one of the social groups that have been most involved in the battle against the pandemic. In fact, society expressed appreciation for their work on social media, and people gathered at the balconies to applaud them. The fact that they felt more valued had positive effects on their mental health (8, 35) and helped them to suffer less (8).
However, the great amount of new negative factors has caused plenty of other negative impacts (Figure 1). Because SARS-CoV-2 is a new virus, doctors have to be constantly updated. Therefore, they have to regularly change their protocols, guidelines, standards or knowledge about the coronavirus. This is confusing and exhausting for them, so it is recommended to have a simpler source of information that could provide them with more security and stability (12). Moreover, the difficult circumstances they have had to face have led them to make decisions that went against their ethical principles, which resulted in significant moral damage (34, 43), shame and guilt (34, 44), or exhaustion and compassion fatigue (34, 45). According to a survey by the British Medical Association (BMA), symptoms of depression, anxiety, stress, fatigue or distress appeared or even worsened among doctors during the pandemic due to the heavy burden that was placed on them (12, 46).
Figure 1. Effects of COVID-19 on the mental health of healthcare workers.

The studies focused on the different specialties of Medicine in order to analyze the consequences. These showed that working on the frontline or in the ICU was an important risk factor for anxiety, but not for depression (8). As for the obstetricians and gynecologists, anxiety and depression levels increased among them during the pandemic (12). In addition, a survey in Spain revealed that 40% of the internists working in direct contact with COVID-19 cases developed symptoms of burnout syndrome. This syndrome is associated with anxiety, depression, substance abuse or the development of psychosomatic symptoms (31). As for psychiatrists, previous research showed that they were already exposed to a number of unique stressors that may increase the risk of deterioration of their mental health (6). However, a study using the CAS revealed that psychiatrists were less anxious than doctors in other specialties. Moreover, psychiatrists coped with the pandemic differently, as they were more reluctant to consider over-information as an effective way of dealing with the pandemic and they were more likely to use sedatives or medication (6). Despite the fact that most studies claim the opposite, a study conducted at the University Hospital Augsburg claims that doctors did not notice changes in their mental health as a result of having direct contact with COVID-19 patients (20).
Besides their specialty and the effects they experienced, it is also important to focus on the fact that the mental health of doctors still remains a taboo. Only very few were able to open up and share their experiences due to fear of how others will react and of being stigmatized. This prevented them from seeking the appropriate support and counselling (12, 47).
- Impact on nurses
Several studies show that the mental health of nurses, whose work has proven to be essential, is suffering considerably. The stress caused by the pandemic is increasing the prevalence of anxiety symptoms (20, 48-50). Some studies claim that this prevalence could have doubled (8, 37). In addition, nursing professionals show more frustration and symptoms of depression due to stress (8, 48), even more than doctors, according to some authors (4, 22).
Researchers from countries severely affected by COVID-19, such as Germany, and from less affected countries, such as Cyprus, agreed that nurses suffered psychologically more than doctors. They showed symptoms that go from anxiety, frustration and depression to a higher level of exhaustion, disenchantment and post-traumatic stress disorder. Furthermore, two other studies suggested that these symptoms might be caused by a closer and longer contact with patients (4, 20), although this contact was not always negative. A study conducted in Andalusia (Spain) indicated that compassion satisfaction among nurses increased due to social recognition and a greater motivation for their patients. Doctors also experienced this, but to a lesser extent (34).
Conclusion
This review collects and analyzes literature about the effects of the COVID-19 pandemic on the mental health of doctors and nurses. In order to do that, we focused on the data obtained from European countries.
Healthcare workers have faced critical situations during the COVID-19 pandemic, which have affected their mental health. They have experienced physical exhaustion due to the long working hours and the moral conflicts they have faced. Facing challenges usually brings out the best in these professionals, but in excess, it can become stressful, draining and exhausting, as seen throughout this paper. This exhaustion does not only affect healthcare workers, but it is also linked with medical errors and other harmful effects for colleagues, patients and the whole health care system (3).
Support from family, friends and the general population is a very effective protective factor, since it provides them with positive reinforcement and a sense of self-efficacy. However, the amount of risk factors over which doctors and nurses have no control is concerning. Furthermore, the early detection of psychological problems helps to identify individuals who are at higher risk in order to act promptly (9). Therefore, it is very important to focus on preventing mental health disorders and break the taboo around them. Protecting the well-being of healthcare professionals is now more important than ever. Helping these professionals will enable them to provide their patients with better care.
Statements
Acknowledgements
The authors of this paper would like to thank the involvement of the coordinating and teaching staff of the “Producción y traducción de artículos científicos biomédicos (III ed.)” and the “Traducción inversa de artículos científicos biomédicos (español-inglés)” courses, as well as the English translation team.
Conflicts of interest
The authors of this paper declare no conflicts of interest.
References
- COVID-19: cronología de la actuación de la OMS [Internet]. World Health Organization; 2021. [Last access: 6 March 2021]. Available at: https://www.who.int/es/news/item/27-04-2020-who-timeline—covid-19
- COVID-19 situation update worldwide, as of week 11, updated 25 March 2021 [Internet]. European Centre for Disease Prevention and Control; 2021. [Last access: 26 March 2021]. Available at: https://www.ecdc.europa.eu/en/geographical-distribution-2019-ncov-cases
- Hummel S, Oetjen N, Du J, Posenato E, Resende de Almeida RM, Losada R, et al. Mental Health Among Medical Professionals During the COVID-19 Pandemic in Eight European Countries: Cross-sectional Survey Study. J Med Internet Res. 2021;23(1):e24983.
- Chatzittofis A, Karanikola M, Michailidou K, Constantinidou A. Impact of the COVID-19 Pandemic on the Mental Health of Healthcare Workers. Int J Environ Res Public Health. 2021;18(4):1435.
- Torrente M, Sousa PA, Sánchez-Ramos A, Pimentao J, Royuela A, Franco F, et al. To burn-out or not to burn-out: a cross-sectional study in healthcare professionals in Spain during COVID-19 pandemic. BMJ Open. 2021;11(2):e044945.
- Jokić-Begić N, Lauri Korajlija A, Begić D. Mental Health of Psychiatrists and Physicians of Other Specialties in Early COVID-19 Pandemic: Risk ind Protective Factors. Psychiatr Danub. 2020;32(3-4):536-48.
- Haravuori H, Junttila K, Haapa T, Tuisku K, Kujala A, Rosenström T, et al. Personnel Well-Being in the Helsinki University Hospital during the COVID-19 Pandemic-A Prospective Cohort Study. Int J Environ Res Public Health. 2020;17(21):7905.
- Buselli R, Corsi M, Baldanzi S, Chiumiento M, Del Lupo E, Dell’Oste V, et al. Professional Quality of Life and Mental Health Outcomes among Health Care Workers Exposed to Sars-Cov-2 (Covid-19). Int J Environ Res Public Health. 2020;17(17):6180.
- Lasalvia A, Bonetto C, Porru S, Carta A, Tardivo S, Bovo C, et al. Psychological impact of COVID-19 pandemic on healthcare workers in a highly burdened area of north-east Italy. Epidemiol Psychiatr Sci. 2020;30:e1.
- Di Tella M, Romeo A, Benfante A, Castelli L. Mental health of healthcare workers during the COVID-19 pandemic in Italy. J Eval Clin Pract. 2020;26(6):1583-7.
- Salazar de Pablo G, Vaquerizo-Serrano J, Catalan A, Arango C, Moreno C, Ferre F, et al. Impact of coronavirus syndromes on physical and mental health of health care workers: Systematic review and meta-analysis. J Affect Disord. 2020;275:48-57.
- Shah N, Raheem A, Sideris M, Velauthar L, Saeed F. Mental health amongst obstetrics and gynaecology doctors during the COVID-19 pandemic: Results of a UK-wide study. Eur J Obstet Gynecol Reprod Biol. 2020;253:90-4.
- Vallée M, Kutchukian S, Pradère B, Verdier E, Durbant È, Ramlugun D, et al. Prospective and observational study of COVID-19’s impact on mental health and training of young surgeons in France. Br J Surg. 2020;107(11):e486-8.
- Dimitriu MCT, Pantea-Stoian A, Smaranda AC, Nica AA, Carap AC, Constantin VD, et al. Burnout syndrome in Romanian medical residents in time of the COVID-19 pandemic. Med Hypotheses. 2020;144:109972.
- Thakrar A, Raheem A, Chui K, Karam E, Wickramarachchi L, Chin K. Trauma and orthopaedic team members’ mental health during the COVID-19 pandemic. Bone Jt Open. 2020;1(6):316-25.
- Rivera-Izquierdo M, Valero-Ubierna M del C, Martínez-Diz S, Fernández-García MÁ, Martín-Romero DT, Maldonado-Rodríguez F, et al. Clinical Factors, Preventive Behaviours and Temporal Outcomes Associated with COVID-19 Infection in Health Professionals at a Spanish Hospital. Int J Environ Res Public Health. 2020;17(12):4305.
- Vanhaecht K, Seys D, Bruyneel L, Cox B, Kaesemans G, Cloet M, et al. COVID-19 is having a destructive impact on health-care workers’ mental well-being. Int J Qual Health Care J Int Soc Qual Health Care. 2021;33(1):mzaa158.
- Mira JJ, Carrillo I, Guilabert M, Mula A, Martin-Delgado J, Pérez-Jover MV, et al. Acute stress of the healthcare workforce during the COVID-19 pandemic evolution: a cross-sectional study in Spain. BMJ Open. 2020;10(11):e042555.
- DiGangi JA, Gomez D, Mendoza L, Jason LA, Keys CB, Koenen KC. Pretrauma risk factors for posttraumatic stress disorder: a systematic review of the literature. Clin Psychol Rev. 2013;33(6):728-44.
- Skoda E-M, Teufel M, Stang A, Jöckel K-H, Junne F, Weismüller B, et al. Psychological burden of healthcare professionals in Germany during the acute phase of the COVID-19 pandemic: differences and similarities in the international context. J Public Health Oxf Engl. 2020;42(4):688-95.
- Zhang W, Wang K, Yin L, Zhao W, Xue Q, Peng M, et al. Mental Health and Psychosocial Problems of Medical Health Workers during the COVID-19 Epidemic in China. Psychother Psychosom. 2020;89(4):242-50.
- Neto MLR, Almeida HG, Esmeraldo JD, Nobre CB, Pinheiro WR, de Oliveira CRT, et al. When health professionals look death in the eye: the mental health of professionals who deal daily with the 2019 coronavirus outbreak. Psychiatry Res. 2020;288:112972.
- Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N Engl J Med. 2020;382(13):1199-207.
- Rothe C, Schunk M, Sothmann P, Bretzel G, Froeschl G, Wallrauch C, et al. Transmission of 2019-nCoV Infection from an Asymptomatic Contact in Germany. N Engl J Med. 2020;382(10):970-1.
- Wang W, Tang J, Wei F. Updated understanding of the outbreak of 2019 novel coronavirus (2019-nCoV) in Wuhan, China. J Med Virol. abril de 2020;92(4):441-7.
- Anxiety on rise due to coronavirus, say mental health charities [Internet]. The Guardian; 2020. [Last access: 26 March 2021]. Available at: http://www.theguardian.com/world/2020/mar/13/anxiety-on-rise-due-to-coronavirus-say-mental-health-charities
- Adams JG, Walls RM. Supporting the Health Care Workforce During the COVID-19 Global Epidemic. JAMA. 2020;323(15):1439-40.
- Lee AM, Wong JGWS, McAlonan GM, Cheung V, Cheung C, Sham PC, et al. Stress and psychological distress among SARS survivors 1 year after the outbreak. Can J Psychiatry Rev Can Psychiatr. 2007;52(4):233-40.
- Pappa S, Ntella V, Giannakas T, Giannakoulis VG, Papoutsi E, Katsaounou P. Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Brain Behav Immun. 2020;88:901-7.
- Salopek-Žiha D, Hlavati M, Gvozdanović Z, Gašić M, Placento H, Jakić H, et al. Differences in Distress and Coping with the COVID-19 Stressor in Nurses and Physicians. Psychiatr Danub. 2020;32(2):287-93.
- Macía-Rodríguez C, Alejandre de Oña Á, Martín-Iglesias D, Barrera-López L, Pérez-Sanz MT, Moreno-Diaz J, et al. Burn-out syndrome in Spanish internists during the COVID-19 outbreak and associated factors: a cross-sectional survey. BMJ Open. 2021;11(2):e042966.
- Xiaoming X, Ming A, Su H, Wo W, Jianmei C, Qi Z, et al. The psychological status of 8817 hospital workers during COVID-19 Epidemic: A cross-sectional study in Chongqing. J Affect Disord. 2020;276:555-61.
- Clavier T, Popoff B, Selim J, Beuzelin M, Roussel M, Compere V, et al. Association of Social Network Use With Increased Anxiety Related to the COVID-19 Pandemic in Anesthesiology, Intensive Care, and Emergency Medicine Teams: Cross-Sectional Web-Based Survey Study. JMIR MHealth UHealth. 2020;8(9):e23153.
- Ruiz-Fernández MD, Ramos-Pichardo JD, Ibáñez-Masero O, Cabrera-Troya J, Carmona-Rega MI, Ortega-Galán ÁM. Compassion fatigue, burnout, compassion satisfaction and perceived stress in healthcare professionals during the COVID-19 health crisis in Spain. J Clin Nurs. 2020;29(21-22):4321-30.
- Wu Y, Wang J, Luo C, Hu S, Lin X, Anderson AE, et al. A Comparison of Burnout Frequency Among Oncology Physicians and Nurses Working on the Frontline and Usual Wards During the COVID-19 Epidemic in Wuhan, China. J Pain Symptom Manage. 2020;60(1):e60-5.
- Liu N, Zhang F, Wei C, Jia Y, Shang Z, Sun L, et al. Prevalence and predictors of PTSS during COVID-19 outbreak in China hardest-hit areas: Gender differences matter. Psychiatry Res. 2020;287:112921.
- Magnavita N, Tripepi G, Di Prinzio RR. Symptoms in Health Care Workers during the COVID-19 Epidemic. A Cross-Sectional Survey. Int J Environ Res Public Health. 2020;17(14):5218
- Shanafelt TD, Gorringe G, Menaker R, Storz KA, Reeves D, Buskirk SJ, et al. Impact of organizational leadership on physician burnout and satisfaction. Mayo Clin Proc. 2015;90(4):432-40.
- Kessler RC, Chiu WT, Demler O, Merikangas KR, Walters EE. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):617-27.
- Braithwaite S, Holt-Lunstad J. Romantic relationships and mental health. Curr Opin Psychol. 2017;13:120-5.
- Wang C, Pan R, Wan X, Tan Y, Xu L, Ho CS, et al. Immediate Psychological Responses and Associated Factors during the Initial Stage of the 2019 Coronavirus Disease (COVID-19) Epidemic among the General Population in China. Int J Environ Res Public Health. 2020;17(5):1729.
- Dush CMK, Amato PR. Consequences of relationship status and quality for subjective well-being. J Soc Pers Relatsh. 2005;22(5):607-27.
- Greenberg N, Docherty M, Gnanapragasam S, Wessely S. Managing mental health challenges faced by healthcare workers during covid-19 pandemic. BMJ. 2020;368:m1211.
- Litz BT, Stein N, Delaney E, Lebowitz L, Nash WP, Silva C, et al. Moral injury and moral repair in war veterans: a preliminary model and intervention strategy. Clin Psychol Rev. 2009;29(8):695-706.
- Winner J, Knight C. Beyond Burnout: Addressing System-Induced Distress. Fam Pract Manag. 2019;26(5):4-7.
- Torjesen I. Covid-19: Doctors need proper mental health support, says BMA. BMJ. 2020;369:m2192.
- Zheng W. Mental health and a novel coronavirus (2019-nCoV) in China. J Affect Disord. 2020;269:201-2.
- Lai J, Ma S, Wang Y, Cai Z, Hu J, Wei N, et al. Factors Associated With Mental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease 2019. JAMA Netw Open. 2020;3(3):e203976.
- Liang Y, Chen M, Zheng X, Liu J. Screening for Chinese medical staff mental health by SDS and SAS during the outbreak of COVID-19. J Psychosom Res. 2020;133:110102.
- Zerbini G, Ebigbo A, Reicherts P, Kunz M, Messman H. Psychosocial burden of healthcare professionals in times of COVID-19 – a survey conducted at the University Hospital Augsburg. Ger Med Sci GMS E-J. 2020;18:Doc05.
AMU 2021. Volumen 3, Número 1
Fecha de envío:
14/03/2021
Fecha de aceptación:
04/04/2021
Fecha de publicación:
31/05/2021